A Guide to Hysterectomy and vNOTES for Arizona Patients
Each year, nearly 500,000 women face the prospect of undergoing a hysterectomy—the surgical removal of the uterus. In some cases, women may also experience the removal of the cervix, ovaries, Fallopian tubes, or other elements of the female reproductive system and its support structures. In the past, this procedure involved the use of either open abdominal surgery or laparoscopic surgery, leaving many women anxious about potential scarring, lengthy recovery times, and other common side effects of traditional hysterectomy surgery.
Now, Arizona Gynecological Consultants is proud to announce the availability of a new, minimally invasive hysterectomy procedure—vaginal natural orifice transluminal endoscopic surgery, or vNOTES. Our own Dr. Heather Zechman has completed advanced training on this highly specialized approach, and since Arizona Gynecological Consultants began offering the procedure in July of 2020, she has performed more vNOTES surgeries than any other surgeon in the state. In addition, Dr. Zechman is one of a select few surgeons in Maricopa County who are highly qualified to perform vNOTES. What is vNOTES? What advantages does vNOTES offer over traditional hysterectomy procedures? Read on to learn more about vNOTES and why it is such a significant advancement in women’s health.

What Is Transvaginal Natural Orifice Transluminal Endoscopic Surgery (vNOTES)?

Transvaginal natural orifice transluminal endoscopic surgery (vNOTES) is an advanced gynecological technique first developed in 2012. While the traditional approaches to hysterectomy—open abdominal surgery and laparoscopic surgery—rely on making one large or
four small incisions into the abdominal cavity, vNOTES avoids abdominal skin incisions altogether. Instead, vNOTES utilizes the vagina as an access path to the uterus and other female reproductive organs and employs innovative technology to improve surgical outcomes. During a vNOTES procedure, the surgeon inserts a vNOTES device known as the GelPOINT® V-Path transvaginal access platform through the vagina and into the pelvic cavity. Then, the vNOTES device inflates the patient’s abdomen with carbon dioxide, giving the surgeon access to the uterus, fallopian tubes, ovaries, and the remainder of the pelvic cavity. The space provided by the device allows the surgeon to both see and operate on the organs inside.
The vNOTES device contains numerous, special openings through which the surgeon can insert the long, thin, surgical tools necessary for a hysterectomy procedure. Also, the surgeon employs the use of a specialized, high-definition camera, which can be inserted through the same access points; the camera allows extensive visualization into the area and allows the utmost precision. Once removal of the uterus is completed, the vNOTES device is removed, and the excess carbon dioxide can escape.
What Advantages Does vNOTES Offer Over Other Types of Hysterectomy Surgery?
As mentioned, the vNOTES procedure does not require any incisions into the patient’s abdominal cavity, instead using the vaginal opening to access the uterus or other reproductive organs.
As a result, vNOTES offers multiple advantages over open abdominal or laparoscopic hysterectomy, including:
- No visible scarring. Since there are no abdominal skin incisions, vNOTES allows the patient to completely avoid the abdominal scarring caused by traditional hysterectomy procedures.
- Shorter operating times. As this efficient procedure does not require creating or closing skin incisions, it takes less time in the operating room than other types of hysterectomy surgery. Traditional hysterectomy surgery can take over three hours, with the average lengths of laparoscopic, other vaginal surgery, and vNOTES requiring much closer to 1 to 2 hours. ? Reduced postoperative pain. Skin incisions and high abdominal pressure are major sources of postoperative pain regardless of the surgery involved. By eliminating skin incisions entirely and reducing the necessary abdominal pressure, vNOTES effectively minimizes the amount of postoperative pain experienced by most women.
- Reduced need for pain relievers. As a direct result of decreased postoperative pain, vNOTES helps to reduce the dosage of pain relievers needed after surgery and can help shorten the length of time they are needed.
- Shorter hospital stays. Unlike other hysterectomy procedures, vNOTES can be performed on an outpatient basis. Research revealed that more vNOTES patients leave the hospital within 12 hours as compared to laparoscopic patients, data that echoes Dr. Zechman’s working experiences. “The vast majority of my patients are able to go home on the same day they were admitted for their vNOTES hysterectomy procedure,” she noted.
- Reduced recovery time. Reduced pain, fewer pain relievers, and shorter hospital stays, coupled with minimal bleeding, mean that vNOTES patients can return to their regular activities much more quickly than either laparoscopic or open surgery patients.
The HALON Study—published in 2019 in BJOG: an International Journal of Obstetrics and Gynecology—affirmed the above advantages of vNOTES. Conducted over two years between 2015 and 2017, this study consisted of a randomized and controlled clinical trial of 70 women, aged 18 to 70, at Imelda Hospital in Bonheiden, Belgium. All were set to undergo hysterectomy for non-cancerous conditions and randomly assigned either vNOTES or laparoscopic procedures. As a result of this study, both the American Association of Gynecologic Laparoscopists (AAGL) and American College of Obstetricians and Gynecologists (ACOG) recommend vNOTES over other procedures whenever possible.
Uses of vNOTES
As vNOTES is a transvaginal procedure—a procedure that takes place via the vaginal opening—it allows surgical access to many of the primary and secondary organs of the female reproductive system. As a result, vNOTES can give surgeons and patients a non-invasive hysterectomy option for the treatment of uterine conditions like uterine prolapse. However, vNOTES provides a non-invasive path for use in other circumstances, as well, including the treatment and removal of uterine fibroids, abnormal bleeding, chronic pain, the removal of adnexal masses, prophylactic ovarian surgery, sterilization, cancer prevention, and more. vNOTES has been successfully employed to perform the following Ob/Gyn surgeries:
- Cystectomy – removal of an abnormal growth or cyst from any of the female reproductive organs
- Salpingectomy – removal of the Fallopian tubes
- Oophorectomy – removal of the ovaries
- Salpingo-oophorectomy – removal of both the Fallopian tubes and ovaries
However, hysterectomy is by far the most common surgery performed using vNOTES, and is one of the most common surgeries experienced by women. Learn more about hysterectomy surgery and what you can expect from the vNOTES procedure in our guide below.
About Hysterectomy Surgery
One out of every nine women will undergo a hysterectomy at some point in her life, making the procedure the second most common type of surgery in women (only cesareans occur moreoften). As a result, obstetrician-gynecologists (Ob/Gyns), gynecologic surgeons, gynecologic oncologists, and general surgeons have dedicated a great deal of research to develop the safest, least-invasive surgical options. Your gynecologist and your gynecologic surgeon can help you determine which option may be best for your situation.
While the average age of a woman undergoing hysterectomy falls between 40 and 45, all women can benefit from reducing the invasiveness of the procedure. As a result, as proven by the HALON study, the least invasive hysterectomy procedure proves to be the best option. Here at Arizona Gynecology Consultants, Dr. Zechman firmly believes in the use of transvaginal natural orifice transluminal endoscopic surgery (vNOTES).
What Conditions Lead to a Hysterectomy?
In part, hysterectomies are so common because they are a practical solution for many gynecological issues after more conservative treatments have failed. Women undergo hysterectomies to treat a variety of conditions, including (but not limited to):
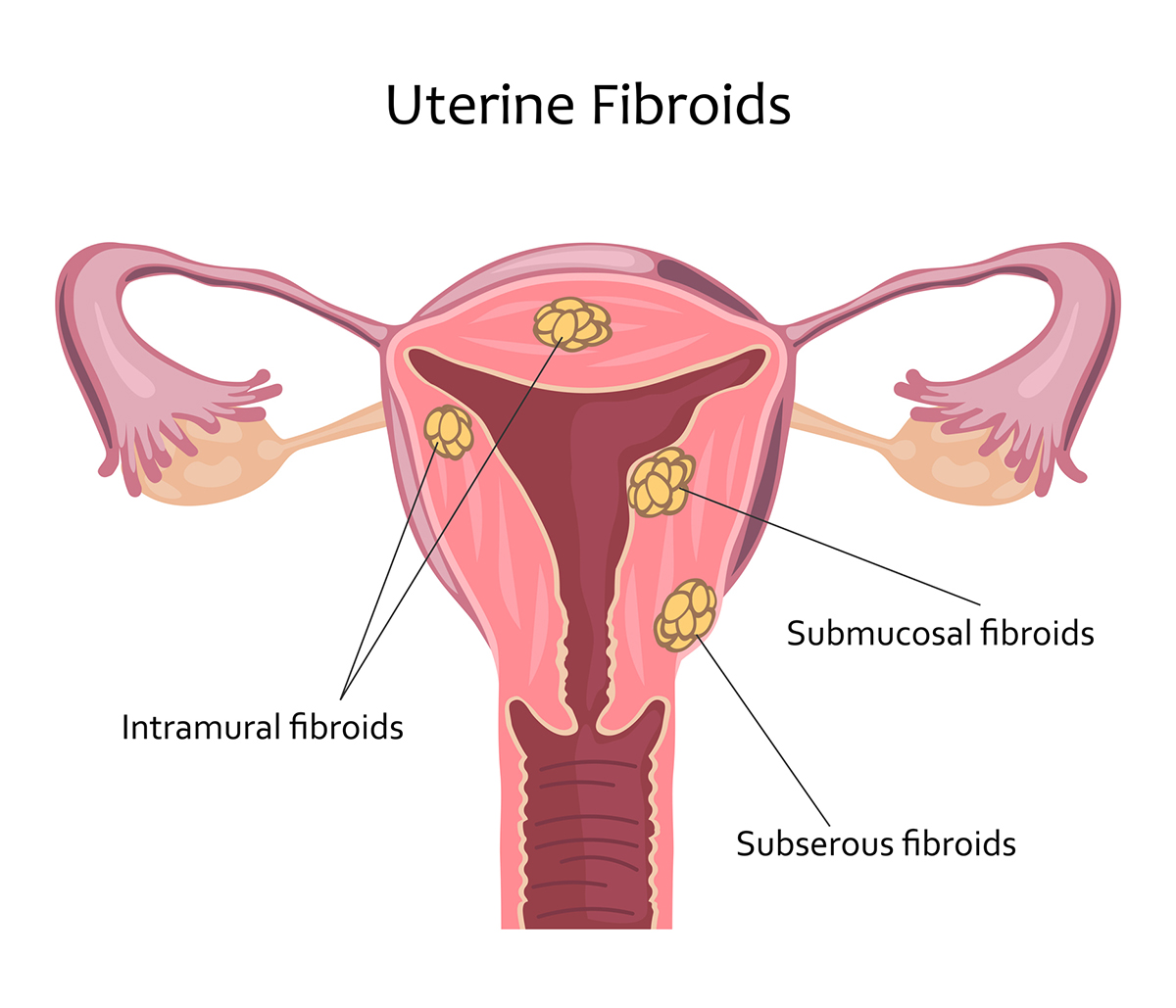
Uterine Fibroids
Uterine fibroids are noncancerous muscular and fibrous tissue growths that protrude from the areas in and around the uterus. Fibroid growths vary in size and typically appear during a woman’s childbearing years; some fibroids may shrink during or shortly after menopause. The cause of fibroids isn’t well understood, though they can sometimes be successfully treated with medications.
Severe fibroids can cause:
- Pain during and after sex
- Painful menstruation
- Excessive menstrual bleeding
- Excessive urination or constipation
In many cases, physicians recommend a hysterectomy to treat severe fibroids that produce heavy, painful bleeding.
Uterine Prolapse
Uterine prolapse occurs when the muscles and ligaments of the pelvic floor are so weakened that the uterus is no longer held in place. In some cases, the uterus slips so severely out of place that it begins to protrude into the vagina.
Most cases of prolapsed uterus are caused by childbirth and can lead to:
- Difficult, painful sex
- Incontinence
- Back pain
If you don’t desire to have any more children, your Ob/Gyn may recommend a hysterectomy to treat a prolapsed uterus.
Pelvic Inflammatory Disease (PID)
Pelvic Inflammatory Disease, or PID, is a bacterial infection of the reproductive system. In most cases, antibiotics are all that’s needed to address the infection; however, if the disease is not discovered early enough, antibiotics may not be sufficient. In these cases, PID can cause extensive damage to the uterus, fallopian tubes, and other reproductive organs and cause additional, prolonged pain. If your PID is causing you severe pain and you no longer wish to have children, hysterectomy may be an option for you.
Cancer

One of the most common reasons for hysterectomy is a cancer of one of the elements of the reproductive system. If you have uterine cancer, cervical cancer, ovarian cancer, or cancer of the fallopian tubes, your oncologist may recommend a hysterectomy. In most cases, hysterectomy becomes an option if cancer is not well-controlled through other methods or if cancer has spread.
Is Hysterectomy an Option for You?
For many women with cancer—especially advanced cancers of the uterus or cervix—a hysterectomy is one of the only options to prevent its further spread. For women experiencing other conditions, however, it is crucial first to determine whether a hysterectomy is the best treatment option.
Discuss the following questions with your physician:
- Are you finished having children, or are you satisfied remaining child-free?
- Are you prepared for the possibility of early-onset menopause?
- Have you attempted other, less-invasive treatment options for your condition?
- Are your symptoms continuing to affect your quality of life negatively?
If you answered yes, hysterectomy is likely a potential solution to your gynecological health issue. However, it’s crucial to note that each case is different and should be evaluated separately. For that reason, it’s important to thoroughly discuss all treatment options with your doctor before deciding on a hysterectomy.
Different Types of Hysterectomy
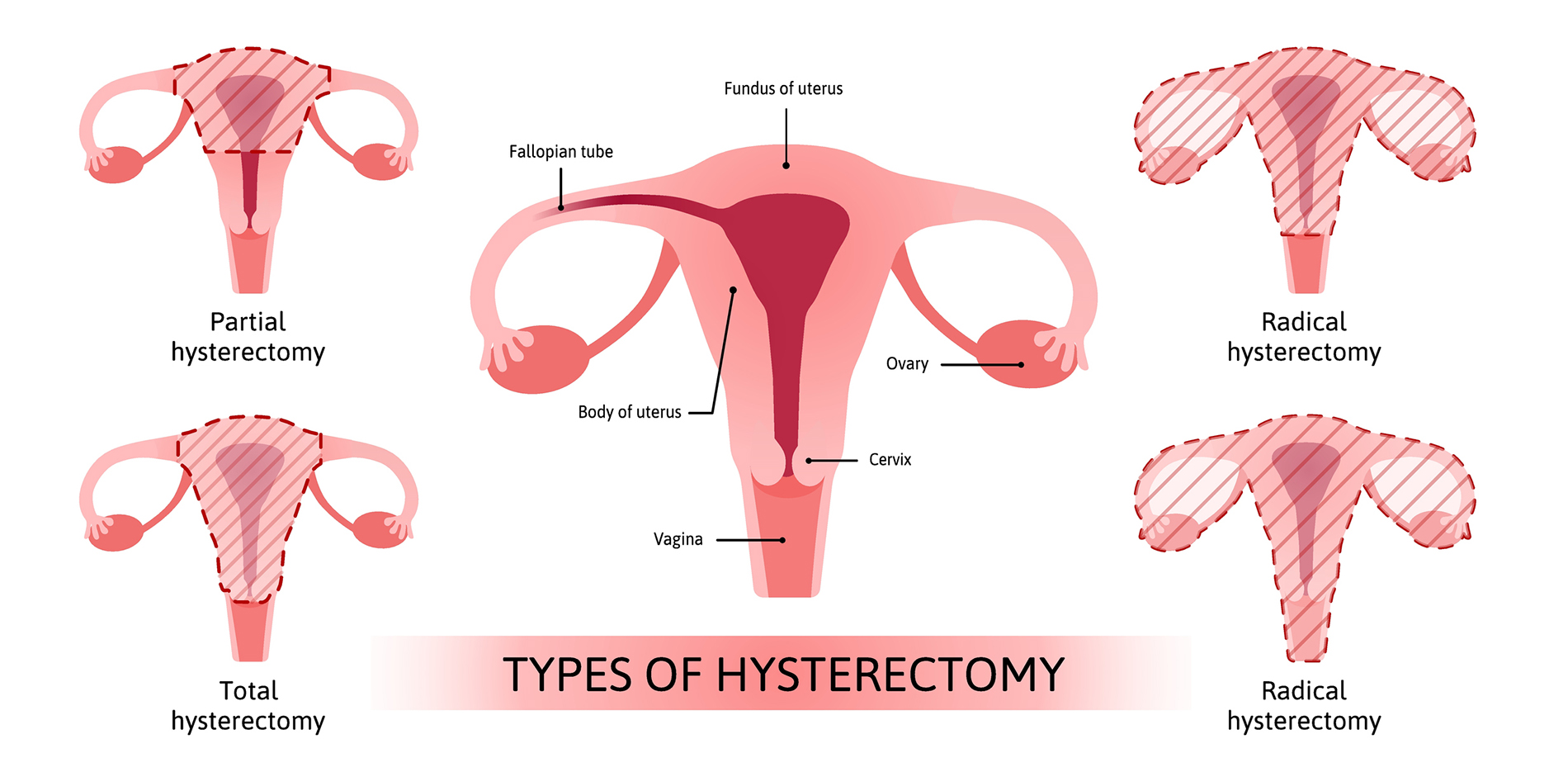
Many conditions may lead to a hysterectomy, and there are multiple types of hysterectomy your physician may recommend. For instance, your physician may recommend the removal of other organs in addition to the uterus—or may want to leave a portion of your uterus as is.
The types of hysterectomy can be broken down into four common categories:
- Complete hysterectomy – this is the type of hysterectomy most people think of when referring to the procedure. In a complete hysterectomy, the surgeon will remove the entirety of the uterus as well as the cervix.
- Partial hysterectomy – in a partial (supracervical) hysterectomy, the surgeon only removes the upper portion of the uterus, leaving the cervix intact.
- Radical hysterectomy – this hysterectomy is the most complete and is usually performed in cases of uterine, cervical, or other cancer. All portions of the female reproductive system are removed, including the uterus, cervix, ovaries, fallopian tubes, upper vagina, and nearby lymph nodes.
- Hysterectomy with bilateral salpingo-oophorectomy – this is the removal of the uterus and both ovaries and fallopian tubes.
Methods of Hysterectomy Surgery
As with most surgical procedures—especially procedures as common as hysterectomy—there are multiple approaches surgeons can take. The type of procedure your surgeon will select depends on his or her skill level, comfort with the procedure, as well as other extenuating circumstances like insurance requirements, hospital scheduling, caseload, available technology, and more. In addition, your surgeon may choose a procedure based on other concurrent procedures you require.
The procedure selected also depends on factors related to your case, such as the condition necessitating the hysterectomy, your symptom severity, and the type of hysterectomy recommended. Factors like the shape of your uterus, the presence of pelvic adhesions, and whether your case is considered emergent can also determine which surgical method is used. Currently, most surgeons in the US rely on one of three surgical methods for hysterectomies.
Traditional Hysterectomy
A traditional hysterectomy—known as an open hysterectomy—requires the surgeon to make a large incision into the abdomen. Typically about five inches, though the size can vary depending on multiple factors, this incision can be placed either vertically or horizontally along the bikini line to minimize scarring on the most visible parts of the abdomen. After incision, the surgeon can view the uterus and the surrounding tissues and remove the uterus and other necessary organs. For particularly large fibroids or a radical hysterectomy, the traditional approach may be necessary for adequate visibility and removal of all the necessary tissue.
Laparoscopic Hysterectomy
As with many modern surgical procedures, surgeons can benefit from the aid of a small camera (or laparoscope) situated at the end of a narrow tool. This camera allows the surgeon to view the interior of the abdomen without making a large incision to expose it. Instead, the surgeon makes multiple, small incisions for the camera and tools and removes the necessary portions of the uterus piece by piece. As the incisions are much smaller, the recovery time is much shorter than from a traditional hysterectomy.
Vaginal Hysterectomy
In a vaginal hysterectomy, the surgeon can avoid making an external incision altogether; instead, a tiny, internal incision is made at the top of the vagina. Using long-handled tools, the surgeon can separate the uterus from its connecting blood vessels and repair any damage. Then, the
uterus (as well as the cervix, fallopian tubes, or ovaries, in some cases) can be removed, piece by piece, through the vaginal canal. This type of hysterectomy makes use of the body’s natural openings and is by far the least invasive type of hysterectomy.
What Is the Best Type of Hysterectomy?

As mentioned, much goes into a surgeon’s decision regarding the type of hysterectomy to recommend. Some conditions may require a traditional hysterectomy due to the sheer size of the uterine fibroid; other surgeons may prefer to perform the type of hysterectomy with which they are most familiar. However, in general, if all else is equal, the best hysterectomy procedure is the one that is the least invasive.
Why? Less invasive surgeries require smaller (or no, in the case of vaginal hysterectomy) external incisions. Utilizing fewer or smaller incisions, particularly through the muscular tissue of the abdominal wall, reduces blood loss during the surgery, minimizes the pain associated with the procedure, and shortens recovery time afterward. Also, fewer complications exist with minimally invasive procedures, reducing your chances of needing to re-enter the hospital or undergo another procedure.
ACOG-Recommended Hysterectomy Procedure [H2] As noted, of the various hysterectomy procedures available today, the American College of Gynecologists and Obstetricians (ACOG), as well as the American Association of Gynecologic Laparoscopists, recommends vNOTES over the others, whenever possible. HALON study research discovered that a vNOTES hysterectomy is just as effective as other methods and offers a superior outcome compared to laparoscopic and traditional hysterectomies. Also, this method is minimally invasive, carries fewer risks, and offers a shorter recovery time than other methods.
Another reason ACOG recommends vNOTES is patient satisfaction. Since this method requires a much shorter surgical time than other methods of hysterectomy and requires less hospital time after surgery, it is also less costly. Also, when surveyed after the surgery and recovery are complete, more patients say they are satisfied with the results of their hysterectomy than patients experiencing either laparoscopic or traditional hysterectomy.
Availability of vNOTES
While the ACOG and gynecologic surgeons alike see the benefits of vaginal hysterectomy over other procedures, the procedure cannot be accessed everywhere. In fact, less than 25% of all hysterectomies are performed vaginally. Two-thirds were performed using the traditional method—despite ACOG support and evidence of better outcomes achieved by vaginal hysterectomy. The reasons for using the method differ, but many surgeons cited lack of training for performing the more effective vaginal method and lack of comfort with the low degree of visibility available in most vaginal hysterectomy surgeries.
This is a set of circumstances especially notable to Dr. Zechman. “Surgical societies see the benefits of minimally invasive vaginal hysterectomy, but the procedure is rarely performed because of the difficulties involved in seeing and accessing critical anatomy. vNOTES solves these challenges using innovative technology designed to enhance patient outcomes,” Dr. Zechman says.
Implementation of vNOTES devices means surgeons can experience greater visibility of the abdominal area necessary for effective hysterectomy surgery. With the device and proper training, more surgeons can perform vNOTES surgery, resulting in a greater overall rate of effectiveness for hysterectomy surgeries.
What to Expect from Your vNOTES Procedure
Like other laparoscopic surgeries, vNOTES takes place while you are under general anesthesia, which means you’ll be asleep during the procedure. A small incision will be made internally, via the vaginal opening, allowing your surgeon to place the special vNOTES device that will provide access to the uterus and any other organs necessary. As with other laparoscopic surgeries, your abdomen will be gently inflated with carbon dioxide to provide room for the procedure.
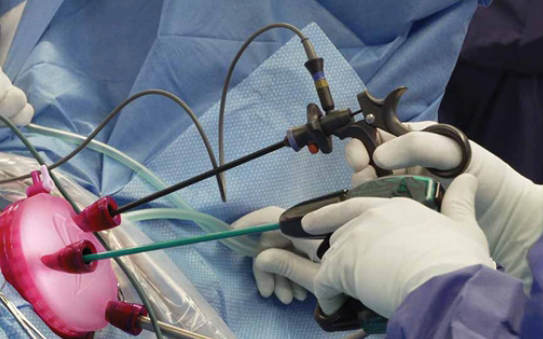
The surgeon will utilize the specially placed openings within the vNOTES device to place a high-definition camera. Using the camera to visualize the area, the surgeon will remove the necessary structures with specialized vNOTES instruments. Once complete, the surgeon will remove the vNOTES device, close the internal incisions, and remove excess carbon dioxide.
In most cases, you’ll be able to return home the same day and will need minimal pain relief for a brief time. Most patients can return to normal activities after two to four weeks and heavy lifting, vigorous exercise, and even sex after about six weeks. However, it is critical that you speak with your physician to determine the appropriate recovery time necessary for your unique case.
vNOTES at Arizona Gynecology Consultants
Arizona Gynecology Consultants is pleased to announce the availability of the minimally invasive vNOTES at our facility. This advanced technique offers many of our hysterectomy patients the option to experience a shorter hospital stay, reduced recovery times, minimal pain, and zero external scarring. Dr. Heather Zechman is a minimally invasive gynecologic surgery (MIGS) specialist and continues to be one of Arizona’s foremost practitioners of this innovative technique.
As with any gynecologic procedure, it is essential to consult with your OB/GYN and Arizona Gynecology Consultants to discuss whether a hysterectomy utilizing vNOTES is right for your condition. We are committed to helping you develop a better understanding of your condition and your treatment options, including vNOTES. Reach out today to see how vNOTES may be a viable option for you.
*Editor’s Note: This article was originally published Sep 29, 2020 and has been updated May 7, 2021.


